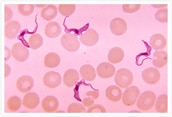
African sleeping sickness (Human African trypanosomiasis) is caused by microscopic parasites of the species Trypanosoma brucei. It is transmitted by the tsetse fly (genus Glossina). As the disease progresses, it causes meningoencephalitis and, eventually, coma and/or death, hence its common name, “sleeping sickness.” It is estimated that 60–70 million people in 36 sub-Saharan African countries are at risk of infection.

Causes of Infection
Also known as sleeping sickness, African trypanosomiasis is caused by a microscopic species of parasites known as Trypanosoma brucei and is spread by the tsetse fly (Glossina). Very rarely, however, infections via mother to child, blood, and sexual activity are also observed.
The two types of African trypanosomiasis are named for the regions in Africa where they were found historically: East African trypanosomiasis (Trypanosoma brucei rhodesiense) and West African trypanosomiasis (Trypanosoma brucei gambiense). Incidentally, West African sleeping sickness mainly infects people, while East African sleeping sickness can infect wild animals and cattle.
Causative Agent:Two parasitic protozoa belonging to Trypanosoma brucei
Vector:Tsetse fly from the genus Glossina
Symptoms
Symptoms in the early stage are relatively mild and may include fever, headache, and muscle and joint pain. However, mental impairment, seizures, and difficulty walking can also manifest in cases where the parasite crosses the patient’s blood-brain barrier and into the central nervous system. If left untreated, the infection worsens, and death may occur in several months to several years.
Both East and West African sleeping sickness are accompanied by the following symptoms. After the first infection, people can be repeatedly re-infected.
West African Sleeping Sickness
Ninety eight percent (98%) of sleeping sickness in Africa is West African sleeping sickness. Early symptoms include lymphadenoma, headaches, intermittent fever, and muscle swelling, none of which are specifically attributable to African sleeping sickness. However, distinct symptoms appear when the infection reaches the central nervous system, including personality change, mental impairment, and seizures. If untreated, it can kill within three years.
East African Sleeping Sickness
East African sleeping sickness accounts for less than 2% of all cases of African sleeping sickness. Normally the disease develops rapidly, showing the first symptoms within a few weeks of infection. In some cases, symptoms may include a large sore (chancre) on the area bitten by the tsetse fly. Unless treated in the early stages of infection, the parasite will invade the central nervous system within a space of few weeks. Death usually occurs within several months.
Diagnosis and Treatment
Diagnostic Methods
For both the West and East African variants, the first step is to conduct blood and other tests. A microscope is used to confirm the presence of the agent. Since it is difficult to discern cases of West African sleeping sickness due to the scarcity of the agent, a lymph fluid test of swollen lymph nodes (posterior neck) and other tests are also necessary. Since different drugs should be administered depending on whether or not the central nervous system is involved, all the patients diagnosed with African sleeping sickness have to undergo a cerebrospinal fluid test.
Treatment
West African Sleeping Sickness
First Stage Treatment
Pentamidine, a drug given intravenously or via intramuscular injection, is used to treat first-stage African sleeping sickness. Suramin is also effective, but since severe adverse reactions can occur in cases where the patient is also infected with Onchocerca volvulus (cause of river blindness), it is not normally used.
Second Stage Treatment (when central nervous system disorders are observed)
Eflornithine, which is administered intravenously four times daily for two weeks, is used to treat second-stage West African sleeping sickness, including in cases where the patient exhibits advanced symptoms of the disease. Although eflornithine is highly effective, it is difficult to administer frequently in clinics and hospitals in rural Africa. For this reason, there has been a tendency to reduce the frequency of eflornithine and, instead, use eflornithine in combination with nifurtimox.
East African Sleeping Sickness
First-Stage Treatment
Suramin is used to treat first-stage East African sleeping sickness. Although suramin can frequently cause adverse reactions, these are usually mild and reversible when the treatment is stopped.
Second-Stage Treatment (when central nervous system disorders are observed)
Melarsoprol is currently the sole drug available for the treatment of second-stage East African sleeping sickness, but adverse reactions to this treatment can be severe and even life-threatening to patients. In 5–10% of patients given melarsoprol will develop an encephalopathic reaction, resulting in a fatality rate of approximately 50%. To reduce the risk of encephalopathy, however, prednisolone can also be administered to patients being treated with melarsoprol. Other adverse effects observed in melarsoprol treatment include skin reactions, gastrointestinal upset and peripheral neuropathy. For these reasons, melarsoprol should be administered with caution.
Prevention
Currently, there is no vaccine or medicine that can prevent African sleeping sickness. Therefore, it is all the more important to avoid contact with tsetse flies. Given the tsetse fly’s characteristic behavior, preventive measures should include not wearing bright-colored or extremely dark-colored clothes, and staying away from bushes where tsetse flies live during daytime.
Regions at High Risk of Infection
Infections of both West and East African sleeping sickness have been reported in rural villages and on the plains of sub-Saharan Africa.
West African Sleeping Sickness
West African sleeping sickness is found in 24 countries in West and Central Africa. More than 95% of cases are reported from the Democratic Republic of Congo, Angola, Sudan, Central African Republic, Chad, and northern Uganda.
East African Sleeping Sickness
East African sleeping sickness is found in 13 countries in eastern and southern Africa. More than 95% of cases are reported from Uganda, Tanzania, Malawi, and Zambia.
Estimated Number of Infected People
There were some 7,000 new cases of African sleeping sickness in 2012. In recent years, the number of reported patients has declined sharply. It is estimated that some 60 million people in 36 sub-Saharan African countries are at risk of contracting African sleeping sickness.
Estimated Number of the Deaths
When left untreated, the mortality rate of African sleeping sickness is close to 100%. It is estimated that 50,000 to 500,000 people die from this disease every year.
References
WHO- Neglected Tropical Diseases, accessed March 19, 2014,
http://www.who.int/neglected_diseases/mediacentre/factsheet/en/
CDC- Neglected Tropical Diseases, accessed March 19, 2014,
http://www.cdc.gov/globalhealth/ntd/diseases/
Editorial Supervisors
Tsutomu Takeuchi, Professor Emeritus of Keio University
Hiroyoshi Endo, Professor Emeritus of St. Luke's International University
