The bite of a rabid dog is the most common way that rabies, an otherwise preventable viral disease of humans and all other mammals, is transmitted. Rabies infection has the potential to threaten over three billion people across Asia and Africa. Although vaccination can prevent rabies, the disease should always be treated immediately after infection. Rabies is nearly always fatal once symptoms develop.
Causes of Infection
Rabies is a preventable viral disease. The rabies virus is most often transmitted through the bite of a rabid mammal. For people, it is usually caused by the bite or scratch of a wild or feral animal, such as a stray dog or raccoon, fox, skunk, or bat. Infection is also possible through contact with the excreta or organs of infected humans and other animals because the virus is contained in saliva as well as in brain and nerve cells.
Agent of the disease:Rabies virus
Reservoir Hosts:Mammals (mainly dogs, foxes, skunks, raccoons, and bats)

Symptoms
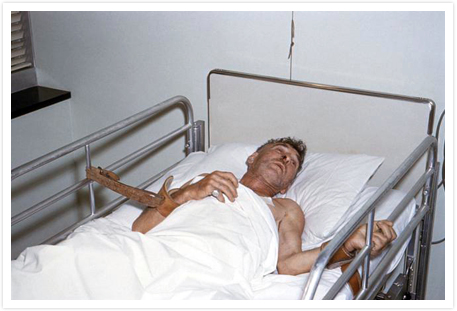
The disease once in the brain results in death. This is because the rabies virus infection has extended to the central nervous system. The early symptoms of rabies in humans include fevers, headaches and general discomfort, and as such these are non-specific and similar to the symptoms of many other illnesses. Pain or unusual unexplained tingling, a prickly feeling, or a burning sensation (paresthesia) are often felt at the site of the wound.
Within three to five days after infection, the virus migrates to the brain from the wound site. This causes more specific symptoms: insomnia, anxiety, confusion, slight or partial paralysis, excitation, hallucinations, agitation, hypersalivation (excessive saliva), difficulty swallowing, and hydrophobia (intense fear of water). Death occurs from cardio-respiratory arrest after several days.
Diagnosis and Treatment
Diagnostic Method
Several specific tests are required to confirm a diagnosis of rabies in humans. The tests that are carried out based on saliva, serum, spinal fluid and/or skin biopsies:
Saliva: Virus isolation or reverse transcription followed by polymerase chain reaction (RT-PCR) is performed.
Serum and spinal fluid: Tests are performed that screen for antibodies of the rabies virus.
Skin: Skin samples are biopsied for the presence of the rabies antigen in the cutaneous nerves.
Treatment
Immediate treatment is required for rabies infections. Quickly applied within several hours after bite, gentle irrigation with water and soap or a dilute water povidone-iodine solution for at least 15 minutes is effective for many kinds of bite wounds and also serves to sharply decrease the risk of infection. After infection, a combination of human rabies immune globulin (HRIG) with a vaccine four times for 14 days is administered. HRIG and the first vaccine should be administered immediately after infection. The vaccine should then be administered on the 3rd, 7th, and 14th days after infection.
If the patient has already been vaccinated, it is enough to give the vaccine on the first and third days of the infection only, without requiring HRIG treatment.
Prevention
Rabies can be prevented with a vaccine. Vaccinating animals that easily carry the rabies virus (mainly dogs) is also an effective prevention method.
Regions at High Risk of Infection
Rabies occurs in more than 150 countries and territories worldwide. However, more than 95% of deaths from rabies are reported to occur in Africa and Asia.
Estimated Number of Infected People
Rabies is a potential threat to over 3 billion people in Asia and Africa. The areas at highest risk are those where people live in rural regions where human vaccines and immunoglobulin are not readily available.
Rabies is most common among children under 15, although people in all age groups can be infected. Each year, more than 15 million people worldwide receive a post-exposure vaccination to prevent rabies. On average, 40% of post-exposure prophylaxis injections are given to both boys and girls from 5 to 14 years old, although the majority is boys.
Estimated Number of Deaths
More than 55,000 people are reported to die of rabies every year, mostly in Asia and Africa.
References
WHO- Neglected Tropical Diseases, accessed March 19, 2014,
http://www.who.int/neglected_diseases/mediacentre/factsheet/en/
CDC- Neglected Tropical Diseases, accessed March 19, 2014,
http://www.cdc.gov/globalhealth/ntd/diseases/
