December 2022
With this disease, people are infected via certain species of mosquito. These mosquitoes carry thread-like worms called filariae that cause a variety of clinical manifestations leading to temporary and permanent disability, including lymphedema of the limbs, genital disease, and elephantiasis (where the legs and/or other body parts swell to resemble those of an elephant). Virtually all patients with lymphatic filariasis also sustain subclinical lymphatic damage. Statistics show that more than 863 million people in 72 tropical and subtropical countries threatened by the disease and 51 million people are infected.
Causes of Infection
Pathogen: Thread-like helminth known as filariae (including Wuchereria bancrofti, Brugia malayi, and B. timori)
Vector: Mainly mosquitoes (Anopheles, Culex and Aedes)
Lymphatic filariasis develops when the filariae transmitted to the human host via a mosquito parasitizes in the lymph system. There are three types of parasite that can be the cause, but it is believed that 90–95% of all lymphatic filariasis is caused by W. bancrofti.
When a mosquito carrying infective filarial larvae bites a person, the larvae enter and migrate within the host’s body. Later, filariae migrate to the lymphatic vessels and develop to the adult stage, causing serious damage to the lymph system. Adult filariae subsequently give birth to thousands of larvae, known as microfilariae, inside the host. These microfilariae are also transferred to the mosquito as it sucks blood, setting off a cycle of further infection. In most cases, childhood infections will continue to develop into adulthood.
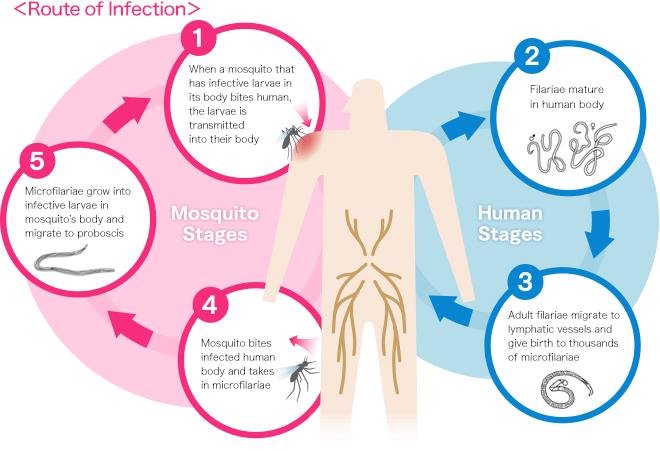
Reference (access August 26, 2022):
U.S. Centers for Disease Control and Prevention, Parasites - Lymphatic Filariasis
Symptoms
During the acute stages of the disease, patients may exhibit characteristic symptoms such as cold chills and spasms commonly associated with fever. Other than these signs, however, there is hardly any indication during the early stages of infection, making many of those infected unaware that they may indeed be afflicted. As infected children grow up, they may experience fever attacks associated with lymphangitis and lymphadenitis, which in time causes circulation lesions of lymph fluid. When the disease develops into chronic conditions, it leads to symptoms such as lymphedema or elephantiasis (tissue swelling and thickening) of limbs and scrotum. In addition to severe pain and permanent disability caused by the disease, it also leads to social stigma associated with the disfiguring visible manifestations. As a result, patients suffer mental, social and financial losses.
Diagnosis and Treatment
Diagnostic Methods
There are two ways to diagnose lymphatic filariasis.
One is verification of the presence or absence of microfilariae in the blood using a microscope. Since microfilariae generally move to peripheral blood at night, blood drawing must be done at night.
The other method is a serological test (antibody titers in blood serum). Regardless of method used, there have been a number of cases where lymphedema has developed several years after a patient was found negative, underscoring the difficulty of accurately diagnosing lymphatic filariasis.
Treatments
Anthelmintics and other drugs for the treatment of lymphatic filariasis include diethylcarbamazine (DEC), albendazole, and ivermectin.
It is possible, however, that lymphedema and elephantiasis continue to develop even after the filariae are destroyed. Basic measures to prevent the symptoms from getting worse include sanitizing the swollen area and exercising to improve the flow of lymph fluid.
Prevention
The most effective preventive measure against lymphatic filariasis is to avoid mosquito bites. It is best to wear long-sleeved shirts and long pants and to apply a mosquito repellent to exposed skin. Mosquito nets over bedding and other sleeping areas are also effective. Once infected with lymphatic filariasis, the patient’s immunity weakens and this leads to susceptibility to other infectious diseases. It is therefore important to maintain hygiene in the home.
To eliminate lymphatic filariasis as a public health problem, the World Health Organization (WHO) recommends community-wide, mass drug administration (MDA) of DEC as well as albendazole or albendazole with ivermectin once a year for at least four to six years in endemic regions. Lymphatic filariasis must also be eliminated from the entire community at once since the disease can be re-transmitted soon after via mosquitoes. Recent evidence shows the combination of above three medicines (triple drug therapy) can safely clear almost all microfilariae from the blood of infected people within a few weeks compared to years using two-medicine regimens. WHO recommends triple drug therapy in areas without onchocerciasis (river blindness) to accelerate the elimination of lymphatic filariasis. (In areas where onchocerciasis is co-endemic with lymphatic filariasis, DEC cannot be administered to communities because of possible side effects that characteristically occur in patients with onchocerciasis).
Regions at High Risk of Infection
The risk of contracting lymphatic filariasis has been confirmed in 72 countries and territories in tropical and subtropical areas of Asia, Africa, the western Pacific, the Caribbean, and Latin America.
Estimated Number of Infected People
More than 860 million people worldwide face the risk of lymphatic filaria infection, with more than 51 million people infected as of 2018.
Worldwide, more than 25 million males have developed genital diseases from lymphatic filariasis and over 15 million patients suffer from lymphedema overall.
Estimated Number of Deaths
While lymphatic filariasis rarely causes death, it weakens the immune system, meaning that patients are also susceptible to other diseases.
References (accessed August 26, 2022):
Editorial Supervisors
Tsutomu Takeuchi, Professor Emeritus of Keio University
Hiroyoshi Endo, Professor Emeritus of St. Luke's International University
