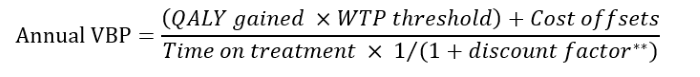- For Print
- June 22, 2022
Eisai Co., Ltd. (Headquarters: Tokyo, CEO: Haruo Naito, “Eisai”) today announced publication of results from an early phase evaluation that aimed to estimate potential economic value of its investigational anti-amyloid-beta (Aβ) protofibril antibody lecanemab in people living with early Alzheimer’s disease (AD) using a validated disease simulation model, AD Archimedes Condition Event (AD ACE) model1,2,3 from the healthcare payer and societal perspectives in the United States, in the peer-reviewed journal Neurology and Therapy. This is the second publication of lecanemab’s potential value. It follows the evaluation of the long-term health outcomes using simulation modeling of lecanemab published in Neurology and Therapy in April 2022.4 While the healthcare payer perspective focuses on direct care costs (e.g., outpatient and inpatient services, medications, intervention costs, nursing home and home healthcare services), the societal perspective further considers societal costs (e.g., productivity loss and informal care costs). As reported in the previous publication, it was suggested that compared to standard of care* (SoC), individuals treated with lecanemab in addition to SoC (lecanemab+SoC) may potentially experience slower disease progression to mild, moderate and severe AD from baseline by 2.51, 3.13 and 2.34 years on average, respectively. The preliminary results of this model-based simulation could possibly translate into additional quality-adjusted life years (QALY**) and reduction in the formal and informal care costs***. Additionally, the AD ACE model framework used in this study allowed assessment of the potential value of lecanemab in different scenarios and sensitivity analyses, including the impact of patient subsets, alternative treatment stopping rules**** and potential dosing regimens as well as major sources of uncertainty.
Eisai is committed to conducting and sharing these types of clinical and socioeconomic analyses to establish trust as we work to potentially bring lecanemab to people living with early AD who have confirmed presence of amyloid pathology in the brain. To that end, Eisai would like to provide a common foundation for stakeholders’ discourse regarding the potential clinical and socioeconomic value of lecanemab from the societal perspective, not to assign a price for lecanemab at this time.
This model-based simulation was conducted using the results of a Phase 2b clinical trial (Study 201) evaluating the efficacy and safety of lecanemab for early AD with confirmed amyloid pathology as well as published literature. It also estimated the potential economic value of lecanemab+SoC over a broad range of willingness-to-pay thresholds from $50,000 to $200,000 per QALY gained as recommended by the Institute for Clinical and Economic Review (ICER)*****. Lecanemab+SoC was predicted to result in a gain of 0.61 QALYs and a decrease in total non-treatment costs of $8,707 per person from the healthcare payer perspective (Societal perspective: 0.64 QALYs gain and $11,214 decrease) compared to the SoC for patients with early AD who have confirmed presence of amyloid pathology. The potential annual value-based price (VBP) of lecanemab was estimated at $9,249 to $35,605 (Societal perspective: $10,400 to $38,053) based on this early economic assessment.
ICER’s value framework5 indicates that value cannot be wholly derived from measures of clinical and cost-effectiveness, so contextual considerations and an examination of other benefits and disadvantages are also added into the framework when assessing long-term value. This may lead to using the societal perspective and higher end of the broad range of willingness-to-pay threshold in estimating the justifiable price of lecanemab, given the large societal burden of AD relative to direct healthcare costs.
Many people living with AD received informal care from their family and friends totaling more than 16 billion hours of unpaid care valued at $271.6 billion in the U.S. in 2021.6 These predicted and simulated findings suggest that early treatment with lecanemab may reduce these costs and economic burdens, and provide insights for healthcare decision-makers regarding the potential clinical and socioeconomic value of lecanemab. The Phase 3 lecanemab Clarity AD data will soon be available to inform the model inputs and refine the findings. In the event that lecanemab receives the U.S. Food and Drug Administration’s (FDA) approval, Eisai may determine a VBP using this framework along with other considerations, such as affordability, health system sustainability, etc.
“Eisai’s goal is to create therapies, such as our investigational anti-amyloid beta protofibril antibody lecanemab, that may help impact the anxieties of people living with Alzheimer’s disease and their families. For Alzheimer’s disease, it is important to evaluate the holistic value of therapies taking into account not only medical costs but also the immense societal costs,” said Ivan Cheung, Senior Vice President, President Neurology Business Group and Global Alzheimer’s Disease Officer, Eisai Co., Ltd., Chairman and CEO, Eisai Inc. “As part of Eisai’s commitment to our human health care mission, trust and transparency, we will continue to publish data and information about lecanemab and look forward to sharing the results of the lecanemab confirmatory Phase 3 Clarity AD clinical trial this fall.”
Eisai completed lecanemab’s rolling submission of a Biologics License Application (BLA) for the treatment of early AD to the FDA under the accelerated approval pathway in May 2022. The Clarity AD Phase 3 clinical study for lecanemab in early AD is ongoing and completed enrollment in March 2021 with 1,795 patients. The readout of the primary endpoint data of Clarity AD will occur in the fall of 2022. The FDA has agreed that the results of Clarity AD, when completed, can serve as the confirmatory study to verify the clinical benefit of lecanemab. Dependent upon the results of the Clarity AD clinical trial, Eisai may submit for full approval of lecanemab to the FDA during Eisai’s fiscal year 2022, which ends in March2023. In Japan, in March 2022, Eisai initiated submission of application data to the Pharmaceuticals and Medical Devices Agency (PMDA) under the prior assessment consultation system with the goal of obtaining early approval for lecanemab, and aims to file for the manufacturing and marketing approval based on the results of Clarity AD during Eisai’s fiscal year 2022. Also, in Europe, based on the results of the Clarity AD study, Eisai plans to submit a new drug application in fiscal year 2022.
This release discusses investigational uses of an agent in development and is not intended to convey conclusions about efficacy or safety. There is no guarantee that such an investigational agent will successfully complete clinical development or gain health authority approval.
* Standard of Care (SoC) for AD currently consists of lifestyle modifications and pharmacologic treatment of symptoms.
** The quality-adjusted life year (QALY) is a measure of the value of health outcomes. Since health is a function of length of life (i.e., quantity) and quality of life (QOL), the QALY was developed as an attempt to combine the value of these attributes into a single index number. One QALY equates to one year in perfect health. QOL scores range from 1 (full health) to 0 (dead). For example, a new intervention may increase length of life by 3 years and improve quality of life by 70% (QALY score of 2.1) compared to an existing intervention that may increase length of life by 3 years and only improve QOL by 50% (QALY score of 1.5), the incremental QALY for this new intervention will be 0.6 QALYs.
*** Formal and informal care costs do not include lecanemab drug cost.
**** Alternative treatment stopping rules were explored in scenario analyses where treatment with lecanemab was stopped after a fixed duration of 1.5, 3 and 5 years.
***** ICER is a non-profit research organization in the U.S. that evaluates the evidence on the clinical and economic value of prescription drugs, medical tests, devices and health system delivery innovations.
1 Kansal AR, Tafazzoli A, Ishak KJ, Krotneva S. Alzheimer's disease Archimedes condition-event simulator: Development and validation. Alzheimers Dement (NY). 2018;4:76-88. Published 2018 Feb 16. doi:10.1016/j.trci.2018.01.001.
2 Tafazzoli and Kansal. Disease simulation in drug development, External validation confirms benefit in decision making. The Evidence Forum. 2018.
3 Tafazzoli A, Weng J, Sutton K, et al. Validating simulated cognition trajectories based on ADNI against 436 trajectories from the National Alzheimer's Coordinating Center (NACC) dataset. 11th edition of Clinical Trials on 437 Alzheimer's Disease (CTAD); Barcelona, Spain: 2018.
4 Tahami Monfared AA, Tafazzoli A, Ye W, Chavan A, Zhang Q. Long-Term Health Outcomes of Lecanemab in Patients with Early Alzheimer’s Disease Using Simulation Modeling. Neurol Ther 11, 863–880 (2022). https://link.springer.com/article/10.1007/s40120-022-00350-y.
5 ICER Value Framework 2020-2023. 2022. ICER_2020_2023_VAF_02032022.pdf
6 Alzheimer's Association. 2022 Alzheimer’s Disease Facts and Figures 2022 Available from: alzheimers-facts-and-figures.pdf.
Media Inquiries:
Public Relations Department,
Eisai Co., Ltd.
+81-(0)3-3817-5120
Eisai Inc. US
Libby Holman
201-753-1945
[Notes to editors]
- 1. About Lecanemab (BAN2401)
Lecanemab is an investigational humanized monoclonal antibody for Alzheimer’s disease (AD) that is the result of a strategic research alliance between Eisai and BioArctic. Lecanemab selectively binds to neutralize and eliminate soluble, toxic amyloid-beta (Aβ) aggregates (protofibrils) that are thought to contribute to the neurodegenerative process in AD. As such, lecanemab may have the potential to have an effect on disease pathology and to slow down the progression of the disease. Currently, lecanemab is being developed as the only anti- Aβ antibody that can be used for the treatment of early AD without the need for titration. With regard to the results from pre-specified analysis at 18 months of treatment, Study 201 demonstrated reduction of brain Aβ accumulation (P<0.0001) and slowing of disease progression measured by ADCOMS* (P<0.05) in early AD patients. The study did not achieve super superiority, which was its primary outcome measure** at 12 months of treatment. The Study 201 open-label extension was initiated after completion of the Core period and a Gap period off treatment of 9-59 months (average of 24 months, n=180 from core study enrolled) to evaluate safety and efficacy, and is underway.
Currently, lecanemab is being studied in a confirmatory Phase 3 clinical study in symptomatic early AD (Clarity-AD), following the outcome of the Phase 2 clinical study (Study 201). Since July 2020 the Phase 3 clinical study (AHEAD 3-45) for individuals with preclinical AD, meaning they are clinically normal and have intermediate or elevated levels of amyloid in their brains, is ongoing. AHEAD 3-45 is conducted as a public-private partnership between the Alzheimer’s Clinical Trial Consortium that provides the infrastructure for academic clinical trials in AD and related dementias in the U.S, funded by the National Institute on Aging, part of the National Institutes of Health, Eisai and Biogen. Since January 2022, the Tau NexGen clinical study for Dominantly Inherited Alzheimer’s disease (DIAD), that is conducted by Dominantly Inherited Alzheimer Network Trials Unit (DIAN-TU), led by Washington University School of Medicine in St. Louis, is ongoing. Furthermore, Eisai has initiated a lecanemab subcutaneous dosing Phase 1 study. Eisai obtained the global rights to study, develop, manufacture and market lecanemab for the treatment of AD pursuant to an agreement concluded with BioArctic in December 2007.
* ADCOMS (AD Composite Score), developed by Eisai, combines items from the ADAS-Cog (AD Assessment Scale-cognitive subscale), Clinical Dementia Rating (CDR) and the MMSE (Mini-Mental State Examination) scales to enable a sensitive detection of changes in clinical functions of early AD symptoms and changes in memory. The ADCOMS scale ranges from a score of 0.00 to 1.97, with higher score indicating greater impairment.
** An 80% or higher estimated probability of demonstrating 25% or greater slowing super superiority in clinical decline at 12 months treatment measured by ADCOMS from baseline compared to placebo.
- 2. About the Calculation of the VBP of Lecanemab
The following can provide a rough approximation of the VBP. The example below is an estimate based on the assumption that a willingness-to-pay (WTP) threshold of $200,000 per QALY gained was used. Different WTP will result in different estimates.
For example, the annual VBP of lecanemab for a WTP threshold of $200,000 per QALY gained from the societal perspective is ($200,000 x 0.64+$11,214) / 3.77 *x 1/(1+3%**) = $38,035. Note that slight change is mainly due to the cost discounting that is applied to treatment cost over time.
* Estimated mean duration of lecanemab treatment calculated by this simulation 3.77 years
** Discounting is a mathematical procedure for adjusting future costs and outcomes of healthcare interventions to “present value”; essentially this means adjusting for differences in the timing of costs (expenditure) compared to health benefits (outcomes). A 3% discounting was considered to estimate the VBP at a WTP threshold of $200,000 per QALY.
- 3. About the Long-Term Health Outcomes of Lecanemab in Early AD Patients
In April 2022, an article about long-term health outcomes of lecanemab in people living with early AD using simulation modeling was published in the peer-reviewed journal Neurology and Therapy. This article describes the comparison of the long-term clinical outcomes for the people living with early AD with SoC alone, and with lecanemab with SoC (lecanemab+SoC), using the disease simulation model (AD ACE model) based on the results of a Phase 2b clinical trial (Study 201) of lecanemab. It was shown that the estimated lifetime risk of disease progression to mild, moderate and severe AD dementia from baseline could potentially be reduced by 7%, 13% and 10% in lecanemab+SoC, respectively, compared to SoC.
In the model, the mean time advancing to mild, moderate and severe AD dementia was longer for patients in lecanemab+SoC group than for patients in the SoC group by 2.51 years (SoC vs. lecanemab+Soc: 3.10 vs. 5.61 years), 3.13 (6.14 vs. 9.27 years) and 2.34 (9.07 vs.11.41 years) respectively and predicted a lower lifetime probability of admission to institutional care in lecanemab + SoC versus SoC group (25% versus 31%). A subgroup analysis by age and disease severity at baseline also revealed a potentially greater impact on disease progression with earlier initiation of treatment with lecanemab. The incremental mean times for transition to mild and moderate AD dementia were 2.53 and 3.34 years, respectively, when treating MCI due to AD in a subgroup analysis compared to SoC. In this simulation analysis or modeling, lecanemab treatment was estimated to potentially slow the rate of disease progression, maintaining treated patients for a longer duration in earlier stages of AD as early AD.
- 4. About the Collaboration between Eisai and Biogen for AD
Eisai and Biogen have been collaborating on the joint development and commercialization of AD treatments since 2014. Eisai serves as the lead of lecanemab development and regulatory submissions globally with both companies co-commercializing and co-promoting the product and Eisai having final decision-making authority.
- 5. About the Collaboration between Eisai and BioArctic for AD
Since 2005, Eisai and BioArctic have had a long-term collaboration regarding the development and commercialization of AD treatments. Eisai obtained the global rights to study, develop, manufacture and market lecanemab for the treatment of AD pursuant to an agreement concluded with BioArctic in December 2007. The development and commercialization agreement on the antibody lecanemab back-up was signed in May 2015.
Our news releases are intended to disclose corporate information and are not intended for the promotion or advertising of prescription pharmaceuticals or investigational products, nor are they intended to provide medical advice.
Please note that the information contained in news releases is current as of the date of publication.